5. Evaluation of the Biological Properties of Chlorin-Type Photosensitizers
Alexander A. Radaev
The «Magic Ray» Moscow Center of Laser Medicine, Moscow, Russia
Introduction
Nowadays tetrapyrrol compounds (like porphyrins and chlorophyll derivatives) attract a lot of interest in connection with therapy of malignant neoplasms. As a result, in the past decade, a special clinical approach was formed. It is called photodynamic therapy (PDT) of tumors which includes consecutive procedures of systemic or local administration of a medicinal compound, called a photosensitizer, into the patient’s body, which is followed by laser irradiation of a tumor at a wavelength which corresponds to one of the absorption peaks of a photosensitizer (as a rule, to a long-wavelength peak). One of the problems of this approach is the increase of selectiveness of photosensitizer accumulation in a tumor, as the consequence of low selectiveness is low efficiency of treatment and enhanced skin photosensibility to day light.
With the purpose to increase this selectiveness, the following methods were used:
- Chemical modification of peripheral substituents of a photosensitizer – a topical and rapidly developing approach in chemistry of tetrapyrrol compounds. The number of published articles on this approach is several hundreds a year.
- Covalent accession of a photosensitizer to monoclonal antibodies against tumor-associated anti-genes.
- Formation of non-covalent complexes of a photosensitizer with lipoproteins.
- Use of liposomal forms of a photosensitizer.
- Delivery by means of vectors able to get selectively bound with bioplasts of cancer cells.
In the sphere of synthetic studies on chemistry of tetrapyrrols, there is a tendency to create compounds with the set properties on the basis of the so-called structurally functional approach. This approach is applicable, in particular, to development and preparation of photosensitizers for PDT of tumors which show high affinity to tumor cells and are more efficient at destroying tumor tissues under irradiation.
Tetrapyrrol compounds as a photosensitizer for PDT of cancer
In 1908 Walter Hausmann was the first to describe in detail the action of hematoporphyrin IX (Figure 1) – a tetrapyrrol photosensitizer made from animals’ blood cells.
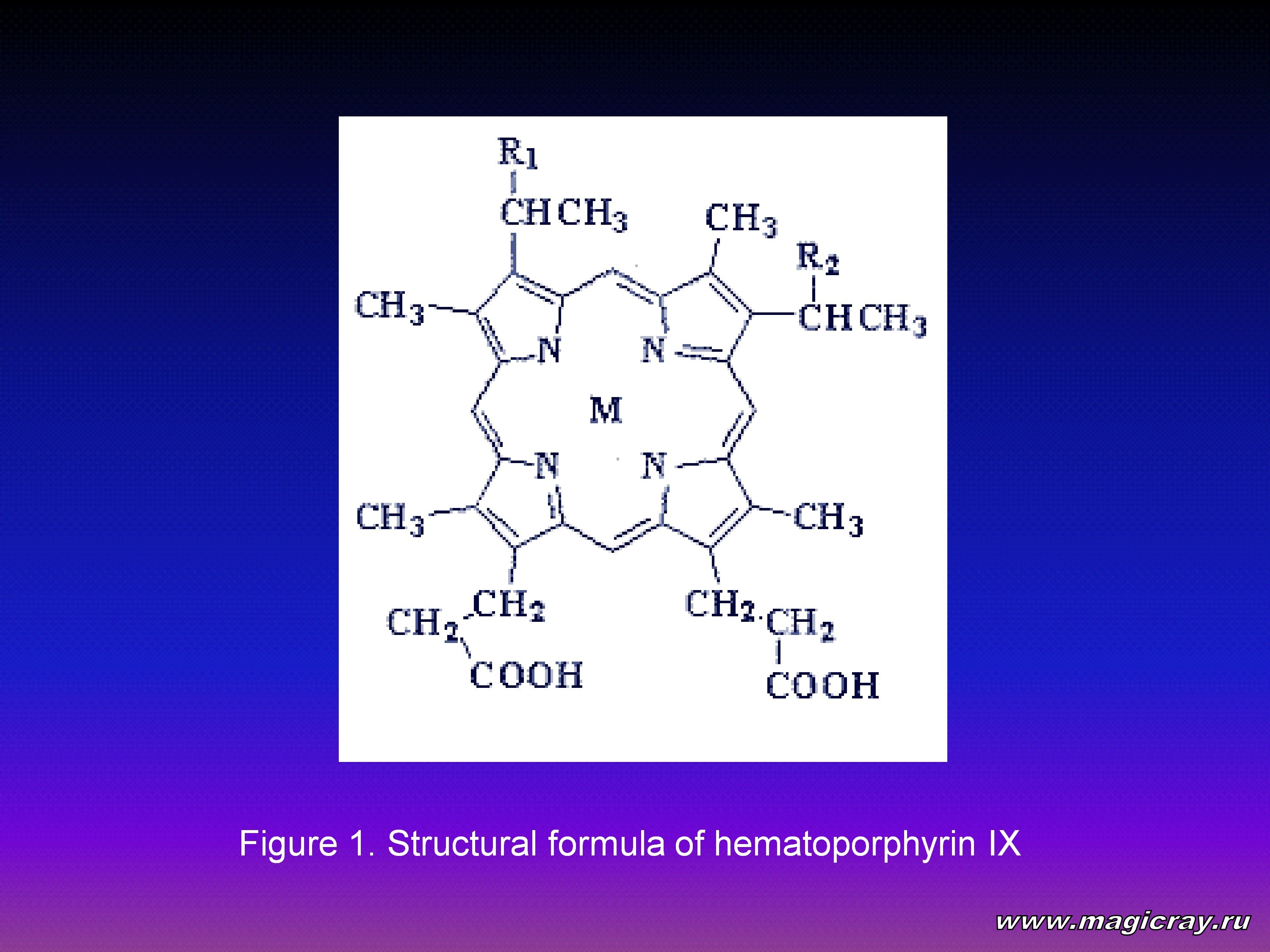
In 1912 Friedrich Meyer-Benz injected hematoporphyrin IX into his body in order to study its biological action. His studies, as well as the studies of his forerunners, did not cause a resonance in the sphere of clinical researches of cancer, but they promoted intensive research of the processes of photodynamic destruction (photodestruction) of cells.
In 1942 Hans Auler and Georg Banzer claimed there was affinity of hematoporphyrin IX to neoplasms, which was confirmed later in the studies by F.H.J. Figge with coauthors (1948), where fluorescence of tumor-associated porphyrins exposed to Wood’s light was discussed. Further development of PDT was generally connected with oligomeric derivatives of hematoporphyrin IX.
In 1977 D.Kessel spoke about in vitro studies of photocytotoxicity of most popular porphyrins (protoporphyrin IX, hematoporphyrin IX, deuteroporphyrin IX, 2,4-diacetyl deuteroporphyrin IX, mesoporphyrin IX). At the beginning of the 1980s, there were synthesized a big number of various 2,4-di (б- alkoxyethyl) derivatives of hematoporphyrin XI. The highest activity was shown by porphyrins which had intermediate polarity, at that their activity increased with the growth of lipophilicity (increase in the size of substituent groups from C1 to C5). It was stated that affinity to tumor cells was influenced by not only the nature of a macrocycle but also by the size of counter ion for anionic photosensitizers. For example, high affinity to tumors was found in some salts of 2,4-di (б-methoxyethyl)-deuteroporphyrin IХ (Dimegin) (Figure 1: R1=R2=ОМе): their accumulation ratio in tumors, in comparison with surrounding tissues, was from 16 to 30. In case with hematoporphyrin IX, this parameter was from 2 to 10.
Among other porphyrin derivatives, a lot of attention in literature was paid to sulphonated derivatives of tetraphenylporphin (TPPSX). From them, researchers were mostly interested in ТРРS4 porphin which contains at the para-positions 4 meso-phenyl substituents of the sulfonate group (R1=R2=R3=R4=РhSО3Н). The first N- alkylated derivatives of meso-tetra(pyridyl)porphin were prepared and used for PDT in vitro.
It was in 1942 when E. Snyder (USA) suggested for the first time that water-soluble chlorophyll derivatives should be used for medical purposes. When administered orally or intravenously, chlorin mixtures, which were mainly composed of chlorin p6 (Figure 2 (1:): R1=Vi, R2=COOH, R3=СООН, R4=СООН), showed low toxicity, hypotensive, antisclerotic, spasmolytic, anesthetic, and antirheumatoid effect. Daily oral administration at a dose of 1 g within 30 days improved the parameters of blood. In particular, the cholesterol level of blood was decreased by 1.5 to 2 times. This fact turned out to be a reason to use water-soluble chlorins to prevent and treat cardiovascular diseases, atherosclerosis, and rheumatoid arthritis.
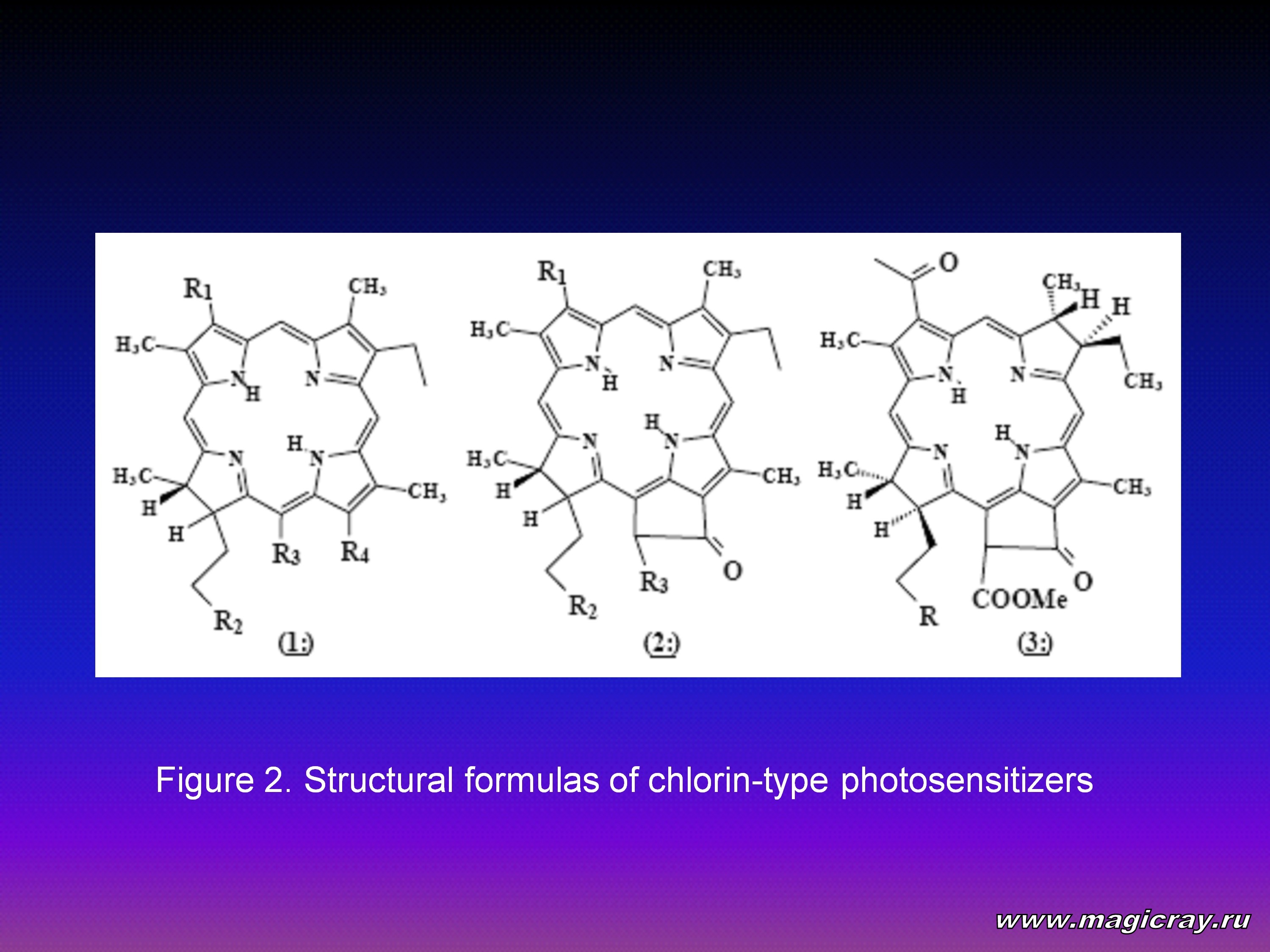
Pheophorbid A derivatives were the first chlorin-type derivatives used in PDT (Figure 2 (2:): R1=Vi, R2=COOH, R3=СООMe). Some of them were patented in 1984 in Japan as potential photosensitizers for PDT (I.Sakata et al.).
The information about the application of chlorin-type derivatives in PDT was first published in scientific literature in 1986, when a group of authors from the USA (J.Bommer, Z.Sveida, B.Burnhem) analyzed the prospects of the properties of chlorin e6 (Figure 2 (1:): R1=Vi, R2=COOH, R3=СН2СООН, R4=СООН), and reported the results of their searches for a photosensitizer which met the most important requirements of PDT, such as good affinity to tumor cells and intensive absorption in the far-red light region. They chose mono-L-aspartyl chlorin e6 (MACE) (Figure 2 (1:): R1=Vi, R2=COAsp, R3=СН2СООН, R4=СООН) which is now undergoing the final stage of clinical trials in Japan. At the same time, J.Bommer and B.Burnhem filed a patent in the USA for the Nippon Petrochemicals Company for a number of functional derivatives of chlorin e6 and bacteriopheophorbid A (Figure 2 (3:): R=COOH) as photosensitizers for PDT.
One of vital tasks of effective PDT realization is the search for a photosensitizer which is able to provide effective usage of this method. As more and more experimental and clinical data appeared, the main requirements to an effective photosensitizer were specified. The requirements included biological (toxic and pharmacokinetic), photophysical and chemical-engineering criteria. First of all, they are:
- low toxicity at therapeutic doses in darkness;
- high selective accumulation in tissues of malignant neoplasms, and rapid elimination of a photosensitizer from the skin and epithelium;
- high absorption in the spectral range where biological tissues have the biggest transmission (the red and near-infrared bands);
- optimum ratio of the fluorescence quantum yield to the interconversion quantum yield, the latter parameter determines the ability of a photosensitizer to generate singlet oxygen (at the same time, the ability of a photosensitizer to fluoresce determines its diagnostic capabilities and facilitates the control of accumulation in tissues and its elimination from them);
- high quantum yield of singlet oxygen production in vivo;
- available manufacturing or synthesis, homogeneous chemical composition;
- high solubility in water or in the allowed intravenous injection solutions, and blood substitutes;
- stability to light exposure and storage stability.
The main restriction of PDT is the penetration depth of laser radiation. Preparations used in clinics have maxima of photodynamic action at 620 to 690 nm. Penetration into biological tissues in this range is very poor, and is only some millimeters. Maximum penetration lies in the far-red and near-infrared bands from 750 to 1,500 nm, and corresponds to the ranges of generation of effective, safe and available lasers. Thus, the production and implementation of photosensitizers which can provide effective generation of singlet oxygen in this range could broaden the sphere of PDT application. Nowadays, such photosensitizers are actively sought among derivatives of chlorins, bacteriochlorins, purpurins, benzoporphyrins, texaphyrins, etiopurpurins, naphthalocyanines, and phthalocyanines. At that, photosensitizers that can be rapidly accumulated in a tumor and show rapid catabolism are of great interest. Eventually, as the history of tumor chemotherapy shows, there will be created a bank of preparations for target spectrum application adapted for specific nosological and histological forms of cancer.
We systematically carry out researches of chlorin-type tetrapyrrol macrocycles (chlorophyll α derivatives) with the purpose to study structural and functional principles of photosensitizer accumulation in a tumor, to enhance therapeutic effect, to create medicinal substances and forms on their basis, to perform overall preclinical analysis of them and implement the best compounds into clinical application of PDT.
Photophysical properties of photosensitizers
As far as compounds which are supposed to show biological activity are concerned, we are, first of all, to examine their photophysical properties in various environments (Table 1).
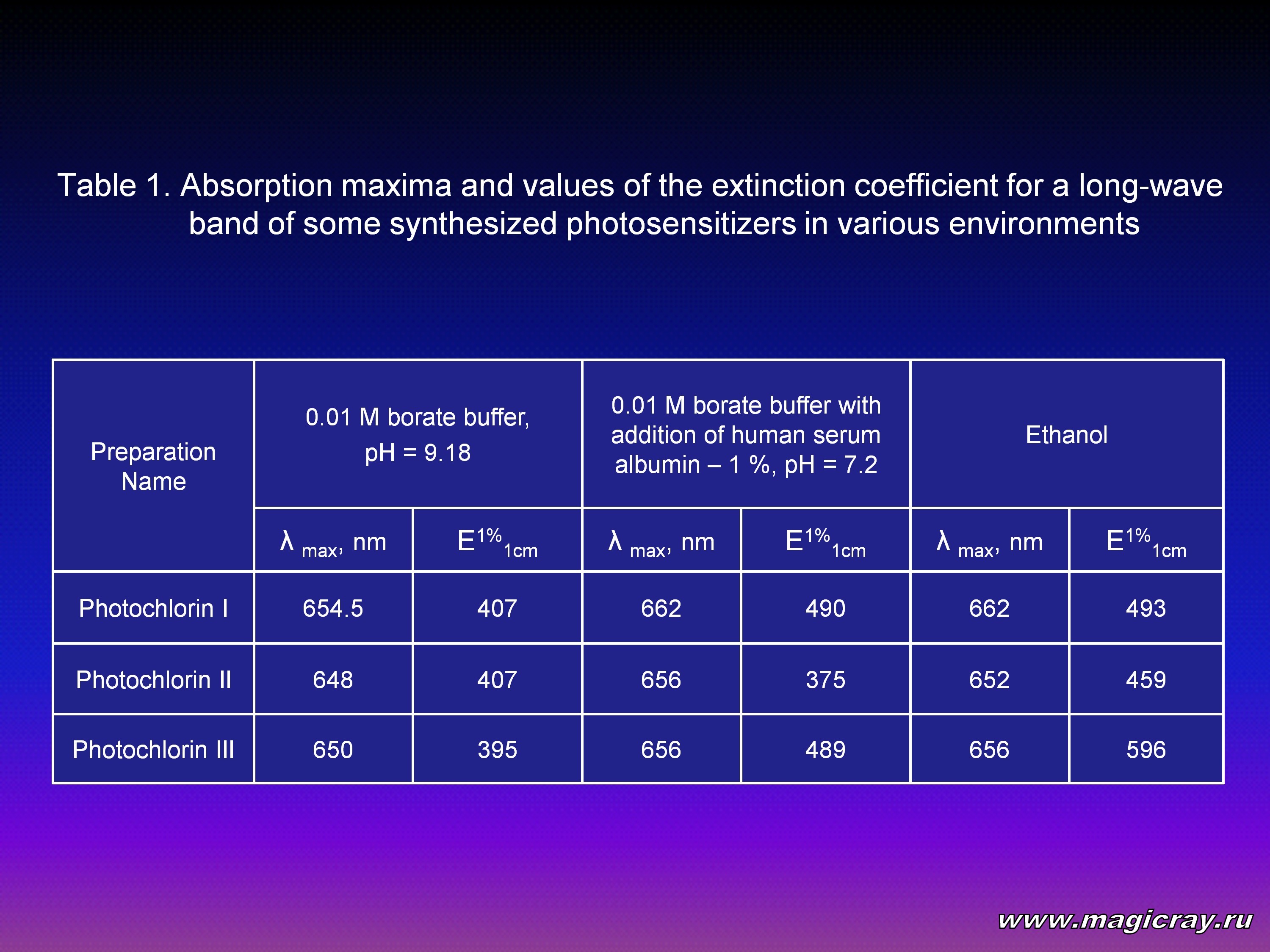
The ability of a substance to generate active toxic factors under irradiation depends on the property of this substance to fluoresce. The lower the fluorescence is, the higher the interconversion quantum yield is, and the higher the photodynamic effect of a photosensitizer is under other same conditions. However, for the purposes of fluorescent diagnostics of tumors with selective accumulation of a photosensitizer in them, it is necessary to maintain in a compound some ability (even a small one) to fluoresce (Table 2).
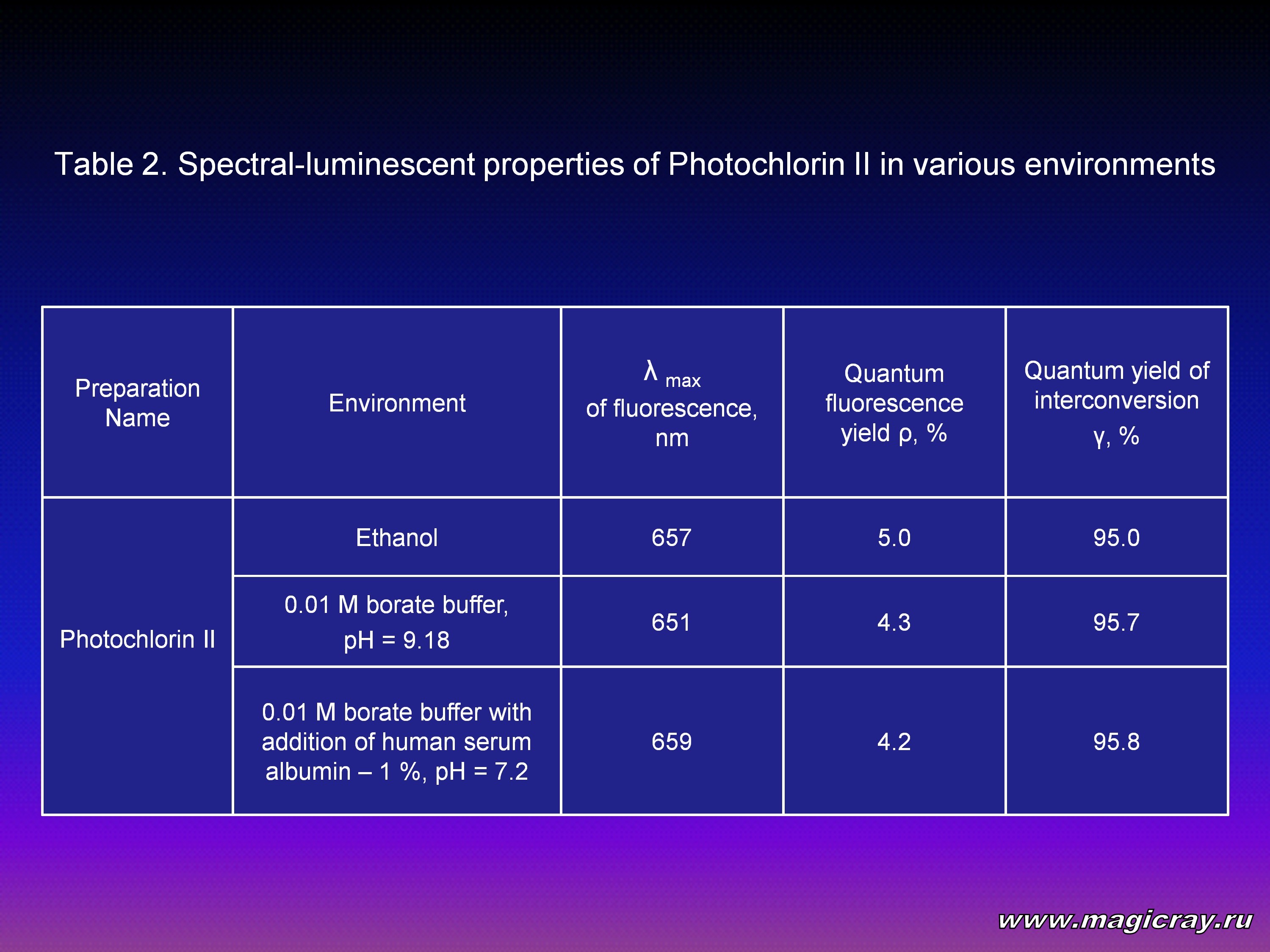
Researching cytotoxicity and cytophototoxicity in vitro
To define if it is possible to use a compound as an effective photosensitizer for PDT, it is necessary to measure its distribution coefficient in the “octanol/buffer solution” system, to evaluate its cytotoxicity and cytophototoxicity in vitro (Table 3).
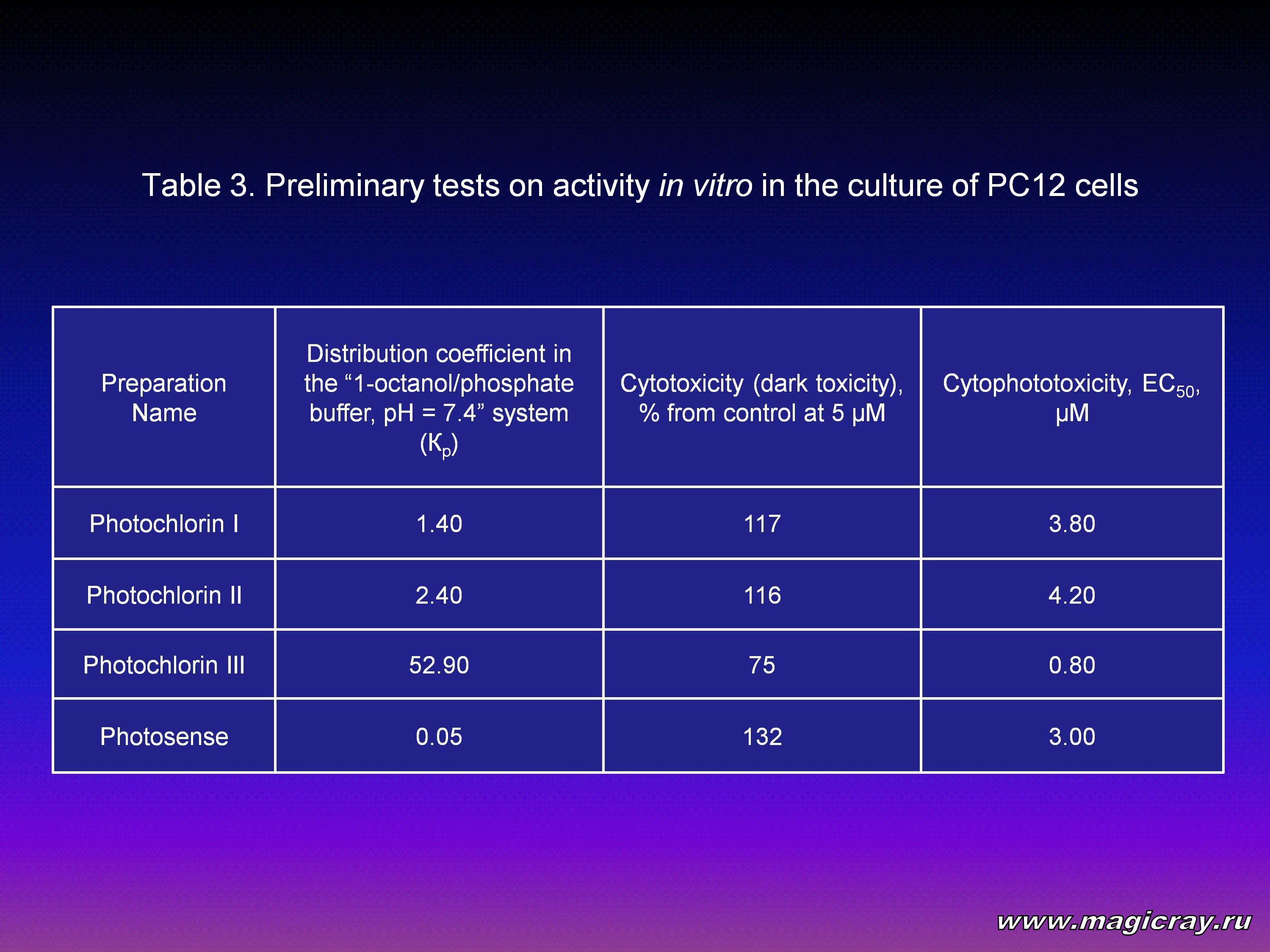
According to the data from literature sources, the highest effectivity as a photosensitizer for PDT is shown by amphiphilic compounds whose distribution coefficient in the “1-octanol/phosphate buffer, рН = 7.4” (Кр) is higher than 1. For synthesized photosensitizers of the Photochlorin series (Table 3), this parameter ranges from 1 to 53, which is a good reason to carry out further researches of the properties of these compounds under condition that they fully maintain their ability to get dissolved in water.
The research of cytotoxic (dark) and cytophototoxic activity of synthesized compounds were performed in the phaeochromocytoma cell culture of a rat (PC12 line) with the usage of an MTT-test as an independent method of evaluation. Photosense (the “NIOPIK” Moscow Science-and-Development Association) was used as a preparation for comparison. The Crystal 2000 (662 nm; 3 W) laser semiconductor device (Russia) was used to excite the photosensitizer, at that, the radiation energy density (the light dose) was 40 J/cm2.
These experiments resulted in the conclusion that Photochlorin I and Photochlorin II slightly, and Photosense significantly enhance cell division, and Photochlorin III, on the contrary, supresses it. Consequently, Photochlorin I, Photochlorin II and Photosense can be expected to produce the effect of tumor growth enhancement under certain conditions, and Photochlorin III to produce a significant cytotoxic effect. However, to make final conlusions it is necessary to carry out researches with the use of several independent methods of evaluation (for instance, with the help of an MTT-test and incorporation of 3H-thymidine into DNA) in at least two or three different cell cultures.
Laser irradiation of a cell culture, incubated with a photosensitizer, causes cell death. Cytophototoxicity of compounds must be evaluated according to the level of effective concentration of a preparation in microMols [μM], 50 % of all cells (EC50) die at this level. In the example given here (Table 3), photosensitizers are ranged according to their effectivity in the following way: Photochlorin III > Photosense > Photochlorin I > Photochlorin II. As far as absolute parameters are concerned, photosensitizers with cytotoxicity lower than 20 μM are believed to be effective.
Acute toxicity and pyrogenity in vivo
Promising results on cytophototoxicity encouraged further researches of preparations with the purpose to evaluate their acute toxicity and pyrogenity in vivo. Researches of toxicity were performed on mice, and of pyrogenity – on rabbits (Table 4), after single intravenous administration of preparations in the form of 0.5 % water solution.
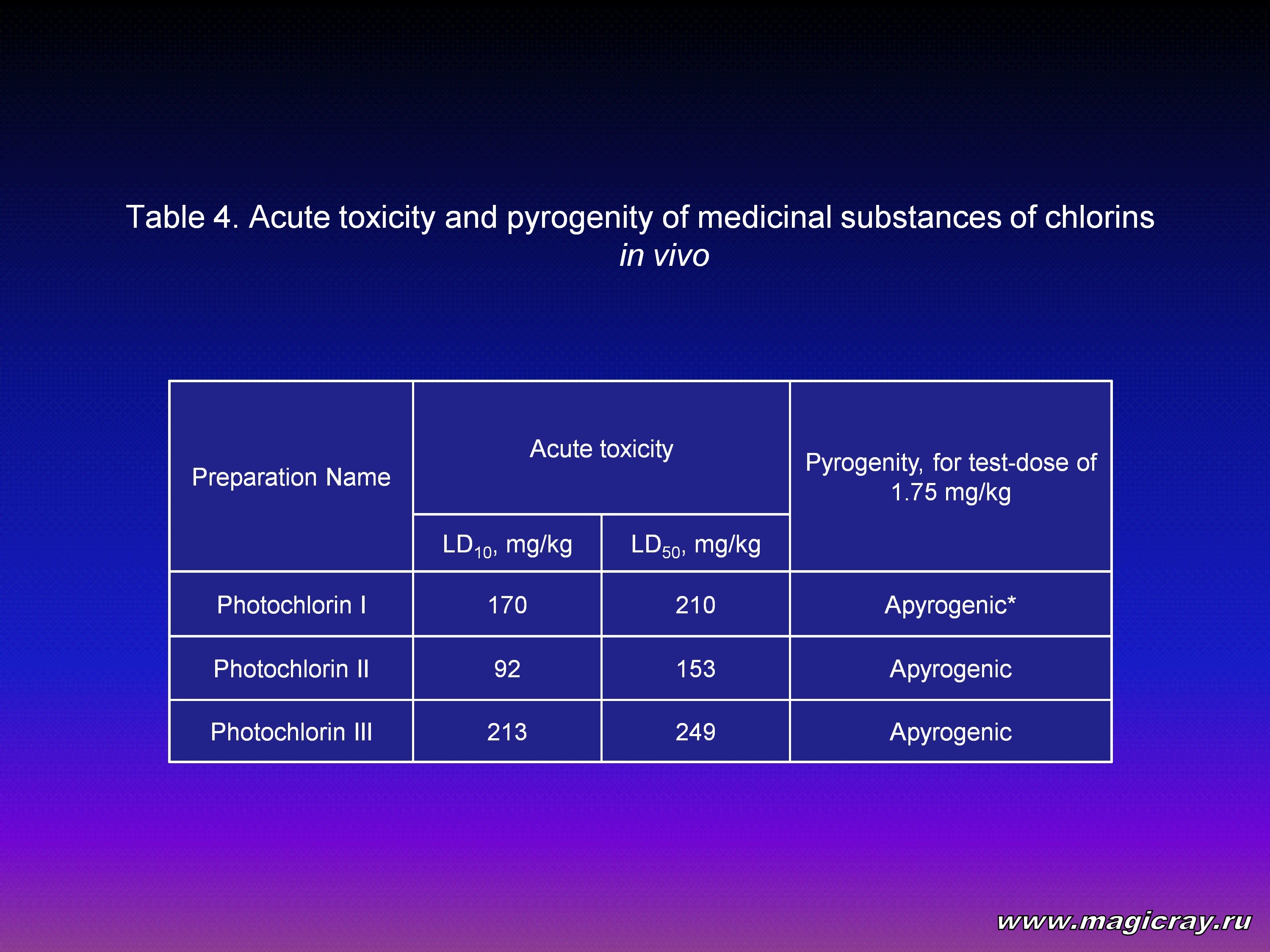
Animals were observed to research acute toxicity. Such parameters were evaluated as: day of death, number of animals which died, clinical picture of intoxication, behavioural reactions, macroscopic condition of internal organs of dead animals. Acute toxicity LD50 was calculated with the help of the method of probit analysis. The obtained results make it possible to refer the photosensitizers under research to the class of “low-toxic” compounds, whose LD50 ranges from 101 to 1000 mg/kg.
During pyrogenity tests, it was stated that Photochlorin II and Photochlorin III are apyrogenic in test-dose of 1.75 mg/kg of rabbit body weight. This test-dose corresponds to the generally accepted doses for pyrogenity determination – 1/20 of a therapeutic dose for a man.
For Photochlorin I, a somewhat higher pyrogenity was fixed. Animals could endure the preparation well and it did not arouse pyrogenity in test-dose of 1.00 mg/kg of animal body weight.
Pharmacokinetics
At intraperitoneal administration of the preparations in doses of 40 mg/kg (Photochlorin I) and 50 mg/kg (Photochlorin II) into mice with embriocarcinoma T36 inoculated into their thigh muscles, the following principles in their distribution are observed. After the administration, the preparations get into the liver, then into blood, and after that they are distributed in animal organs and tissues (Table 5). After single intravenous administration of the preparations in the form of 0.5 % water solution, the maximum level of their accumulation in a tumor is achieved 30 minutes later after the administration.
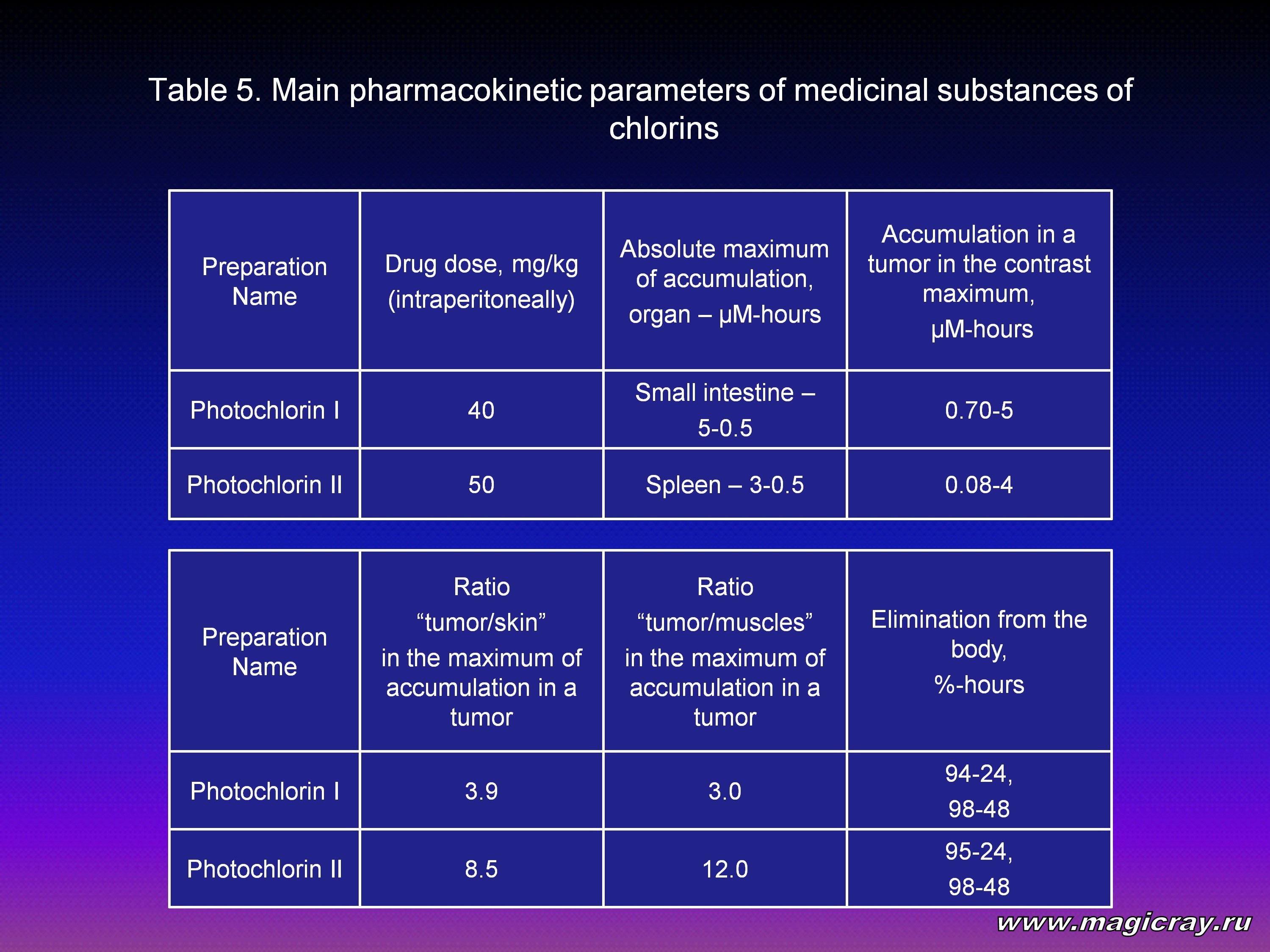
A differential peculiarity of the Photochlorin I distribution in organs is its significant accumulation in the small intestine – by 2.5 to 5 times as much as in other organs. However, this process is short-time, and 18 hours after the administration the concentration in the small intestine decreases by a factor of 100. The contrast index (ratio of the concentration in a tumor to the concentration in surrounding normal tissue) is 3 to 4. Maximum differences could be fixed 5 hours after the administration of a preparation.
A differential peculiarity of the Photochlorin II distribution in organs is its rapid accumulation in the spleen – by 10 to 30 times as much as in other organs. Two hours later the preparation gets distributed in the liver and kidneys, and 4 hours later – in small intestine and blood. However, this process is short-time, and 8 hours after the administration the concentration of the preparation in organs and tissues decreases more than one order. The contrast index (ratio of the concentration in a tumor to the concentration in surrounding normal tissue) is 8 to 12. Maximum differences could be fixed 4 hours after the administration of a preparation. A drawback of this compound is that when it is administered intraperitoneally, it is strongly kept in tissues of the abdominal cavity, which makes absolute parameters of accumulation in a tumor not very high. Probably, this drawback will not be of great importance for intravenous administration.
The main way of preparations elimination from the body is through the intestine. Kidneys also contribute to the elimination of compounds from the body. The biggest quantity of the administered dose is eliminated within the first 24 hours. Photosense, the preparation which is used nowadays, remains present in the body within more than 90 days, which causes significant difficulties in its usage because of the risk of light stress.
The obtained data make it possible to suggest that the ideal time to perform PDT with the usage of Photochlorin I and Photochlorin II is 5 and 4 hours after administration, respectively.
Researching photodynamic activity of Photoditazine in experiments of in vivo
The researches were carried out with the purpose to find the conditions which would be most effective for conducting photodynamic therapy with Photoditazine – chlorin e6 derivative. Photodynamic activity of Photoditazine in in vivo experiments on animals which had tumors was analyzed depending on the dose of the preparation (drug dose) and the dose of light energy given to a tumor (light dose).
Photoditazine is N-dimethylglucamine salt of chlorin e6, a compound with a good ability to get dissolved in water with an intensive absorption maximum in the spectral region of 662 ± 5 nm. This photosensitizer is of plant origin and was made on the basis of chlorophyll б derivatives produced from the biomass of Spirulina platensis Gom. Geitleri microalgae.
The researches were carried out on 270 outbred rats weighing 130 to 150 g and 20 mice weighing 20 to 22 g which were inoculated subcutaneously into their thigh muscles with: M1-sarcoma, breast tumor, B16-melanoma. Animals were brought to experiment 7 – 10 days later after the day of inoculation. Photoditazine was administered intraperitoneally at drug doses of: 0.5; 2.5; 5.0; 10.0 mg/kg. The procedure of irradiation was performed with the help of the Crystal 2000 (662 nm; 3 W) laser semiconductor device (Russia). Before the procedure the hairy area of tumor growth was depilated, and the animals were given ether anesthesia. Irradiation was performed 2.5 – 3 hours later after the administration of Photoditazine. Each animal underwent a single procedure of irradiation at an average light dose: 150, 200, 300, 400, 600 J/cm2.
The photodynamic effect of Photoditazine was analyzed on the 3rd, 7th, 10th, 14th, 21st days after PDT according to the coefficient of absolute tumor growth (C) and the effect of tumor growth inhibition (Guidelines of the Pharmaceutical Committee on pre-clinical tests of preparations, 2000).
To analyze the effectivity of tumor growth inhibition, they calculated an average tumor volume in experimental and control groups of animals. The level of tumor growth inhibition was determined according to the index of tumor growth inhibition (TGI) which can be calculated with the help of the following formula:
TGI = [(Vcontrol –Vexperimental)/Vcontrol] x 100 %,
where V is an average tumor volume (cm3) in experimental and control groups of animals, respectively.
Besides TGI, the parameter of complete tumor regression (CTR, %) was used to determine a quantitative criterion of evaluation of the inhibiting effect.
Quantitative criteria of evaluation of the inhibiting effect:
| TGI < 20 % |
|
0 |
| 20 % ≤ TGI < 51 % |
|
+– |
| 51 % ≤ TGI < 81 % |
|
+ |
| 81 % ≤ TGI < 91 % |
|
++ |
| (91 % ≤ TGI ≤ 100 %) + (CTR < 50 %) |
|
+++ |
| (91 % ≤ TGI ≤ 100 %) + (CTR ≥ 50 %) |
|
++++ |
Photodynamic therapy of B16-melanoma
The specific activity of Photoditazine 0.5% solution was researched on 16 mice weighing 20 to 22 g which were inoculated subcutaneously with B16-melanoma into their thigh muscles of a hindfoot. Photoditazine at doses of 5 mg/kg and 10 mg/kg was administered intraperitoneally 2.5 hours before the procedure of irradiation. The animals under anesthesia were exposed to irradiation with the help of the Crystal 2000 laser semiconductor device (Russia): the wavelength (λ) was 662 nm; radiation power density (P) was 0.35 W/cm2; light energy dose (E) was 200, 300, 400 J/cm2. The dynamics of B16-melanoma growth is given in Table 6.
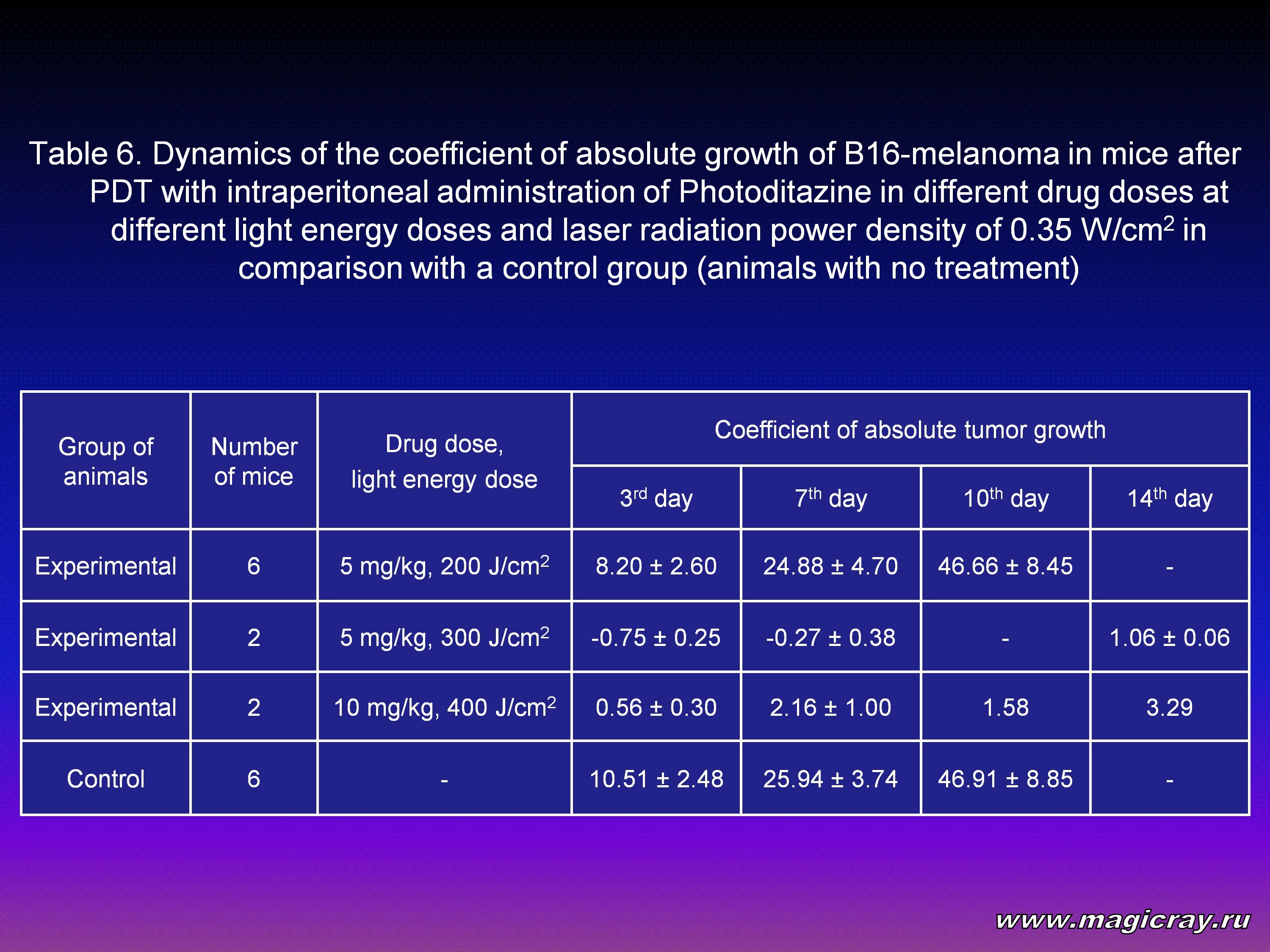
The Table shows that by the 14th day after the inoculation, mice with B16 melanoma in the control group start to die. After PDT (5 mg/kg; E = 200 J/cm2) the dynamics of tumor growth was the same as in the control group. Increase of a light energy dose up to 300 J/cm2 stimulated significant inhibition of melanoma growth. At that, the coefficient of absolute tumor growth on the 14th day was nearly 1, and in the control group on the 10th day it was 46.91. A high level of melanoma growth inhibition in mice is proved by the results obtained after the administration of Photoditazine at a dose of 10 mg/kg and irradiation of a tumor at a light dose of 400 J/cm2. The results of the experiments performed on melanomas in mice show a high specific activity of Photoditazine.
Photodynamic therapy of breast tumor
The results of PDT performed on breast tumor in rats (Table 7) show significant inhibition of tumor growth after photodynamic therapy in comparison with the control group.
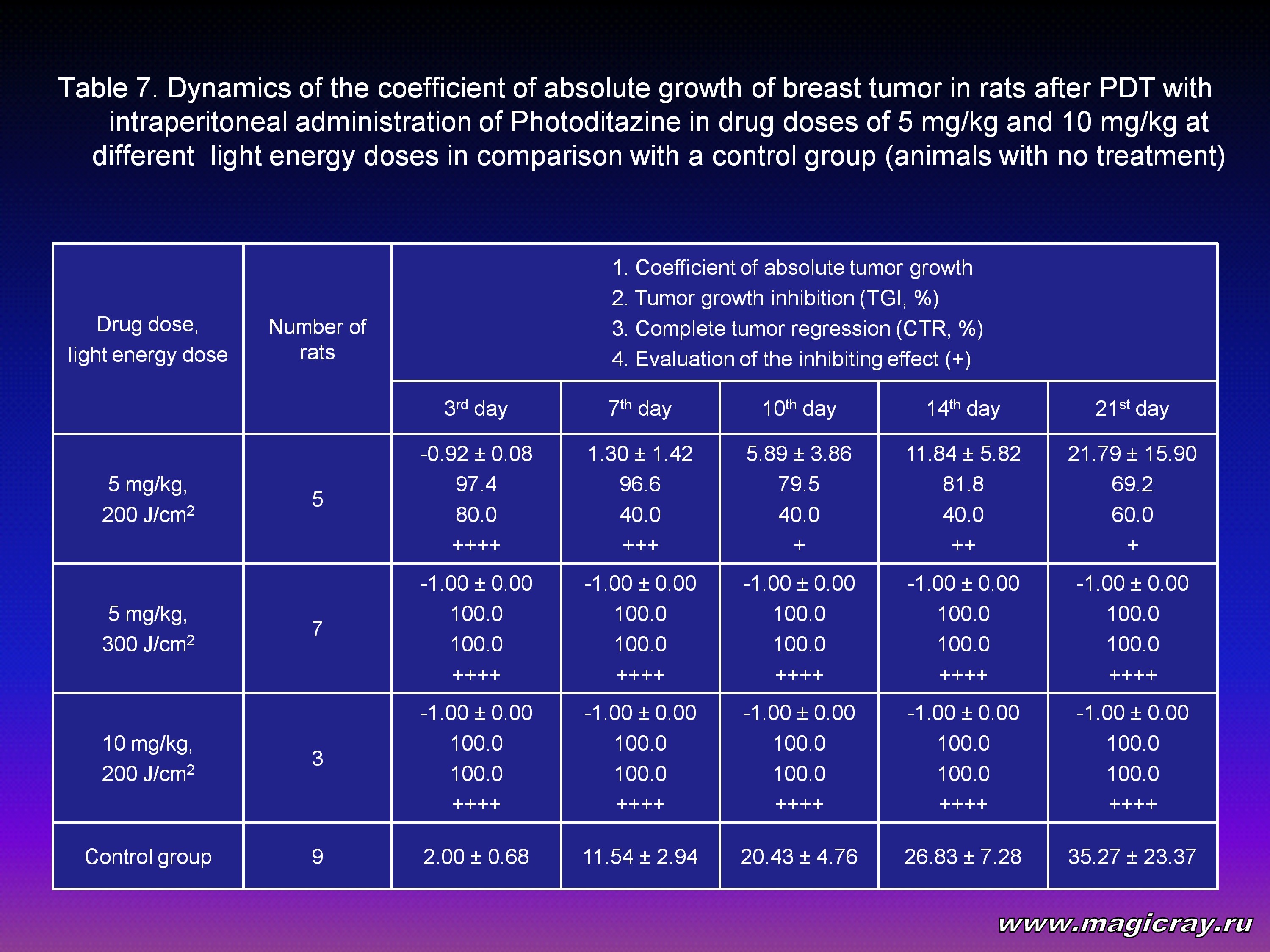
The tumor volume in the group of animals, which were injected intraperitoneally with Photoditazine at a dose of 5 mg/kg (E = 200 J/cm2) 2.5 hours before the procedure of irradiation, reduced on the 14th day from 97 % to 82 %. On the 21st day the parameter of tumor growth inhibition in this group reduced to 69 %, but the parameter of complete tumor regression increased up to 60 %.
A doubled dose of Photoditazine (up to 10 mg/kg) with the same light dose (200 J/cm2) or increase of a light dose up to 300 J/cm2 with the same dose of the preparation (5 mg/kg) resulted in 100 % breast tumor regression.
Photodynamic therapy of M1-sarcoma
Laser irradiation of M1-sarcoma was performed 2.5-3 hours later after intraperitoneal administration of Photoditazine at doses: 2.5 mg/kg (Tables 8-1, 8-2), 5 mg/kg (Tables 9-1, 9-2), 10 mg/kg (Table 10).
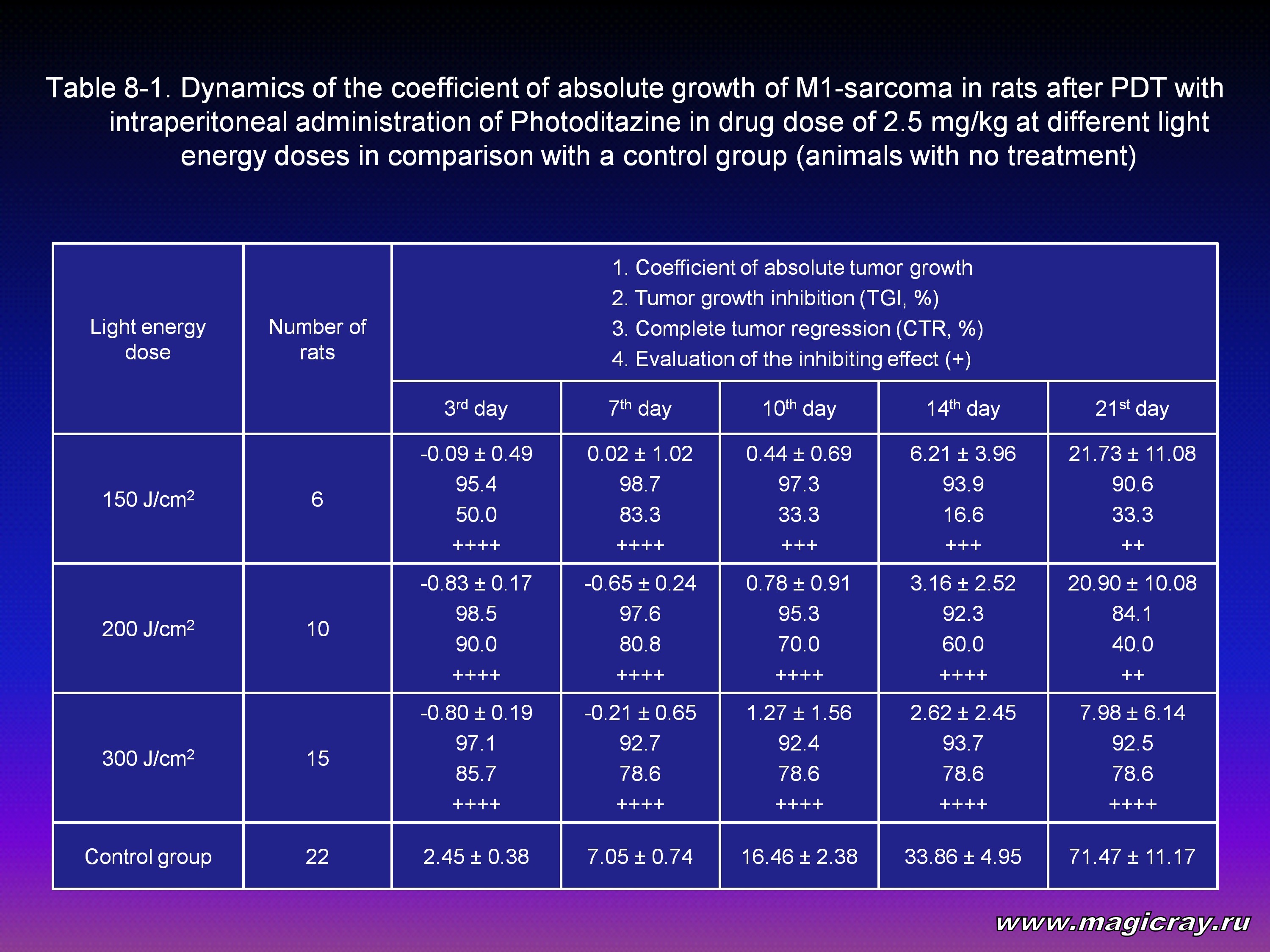
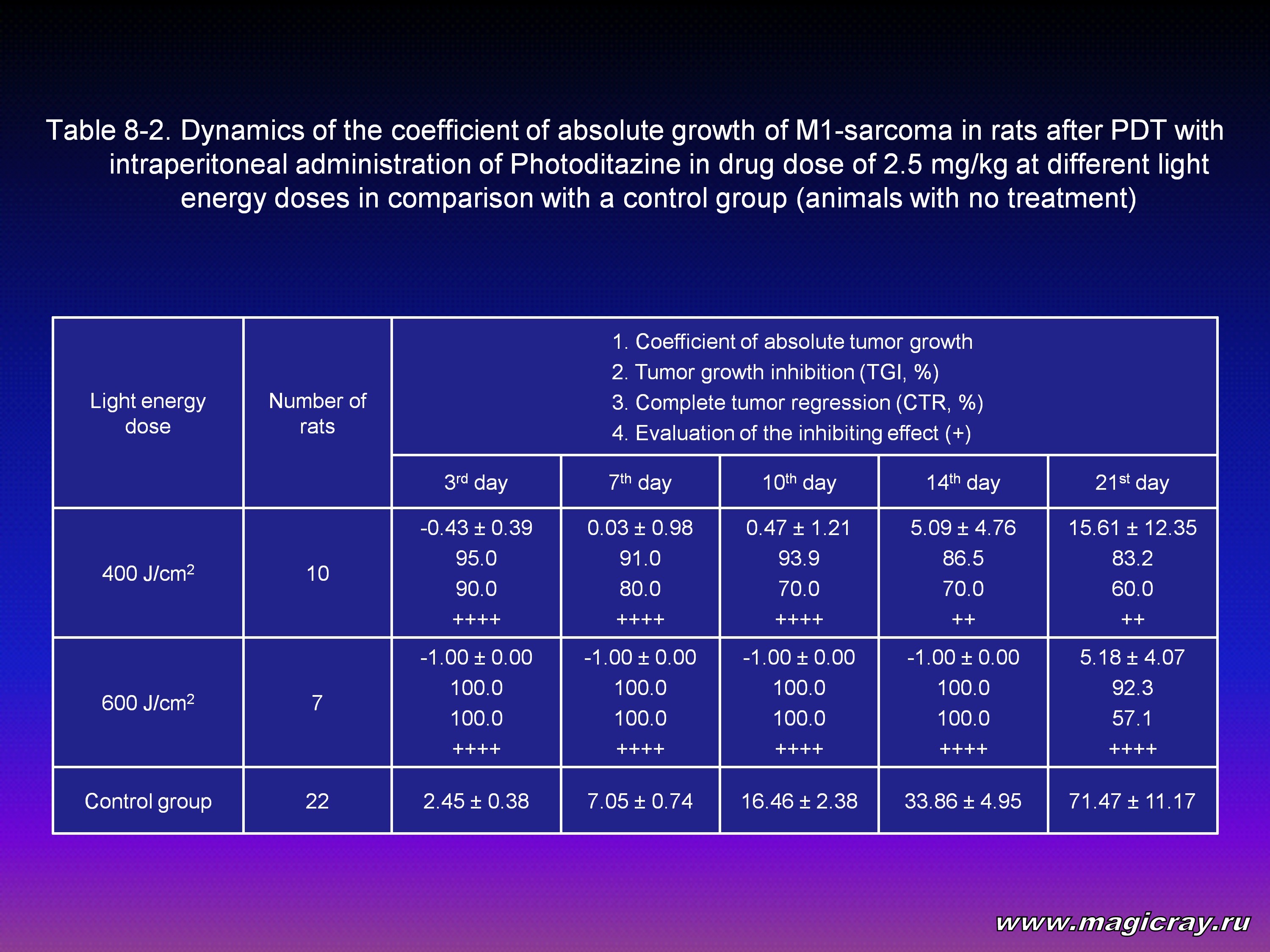
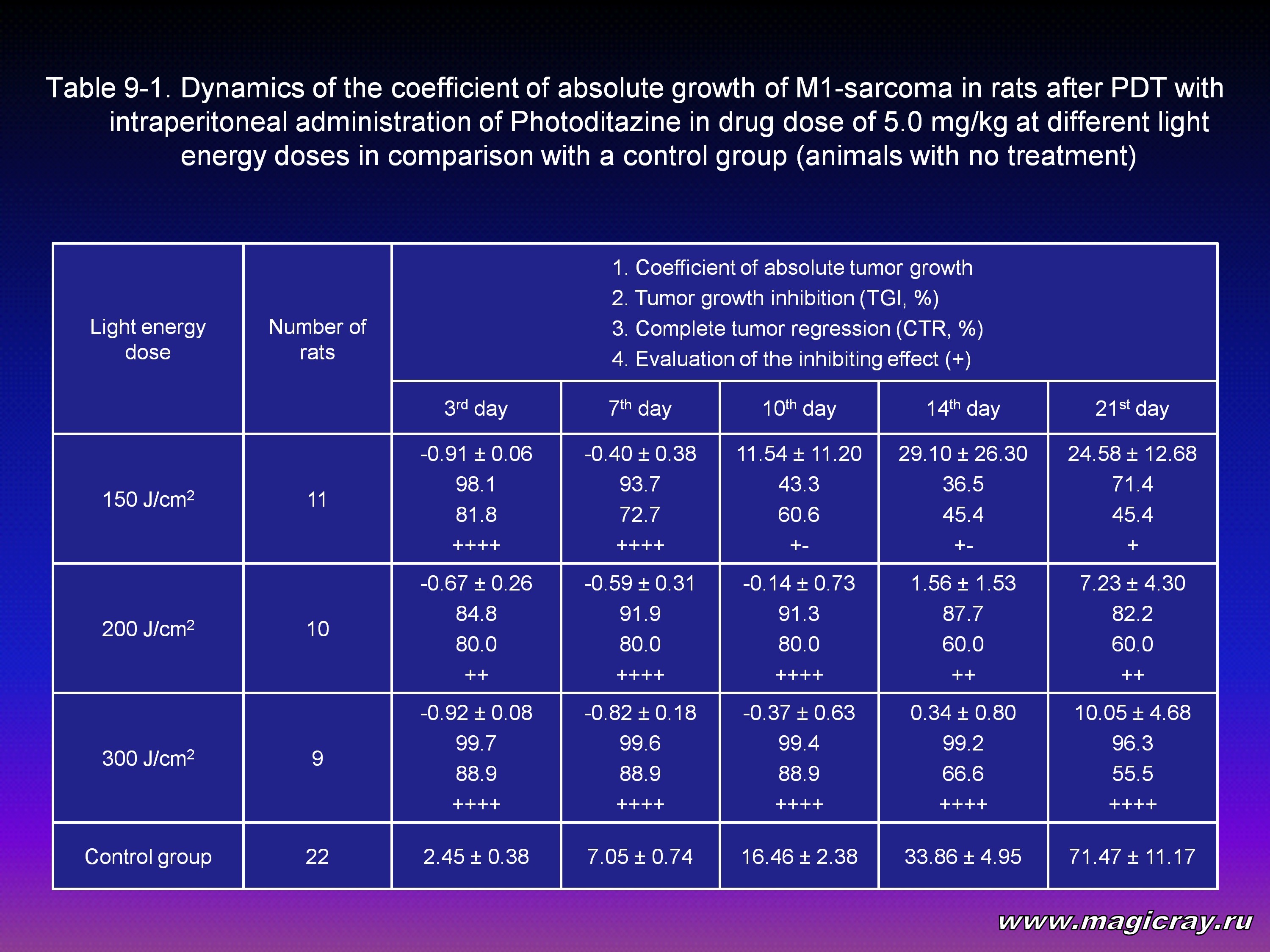
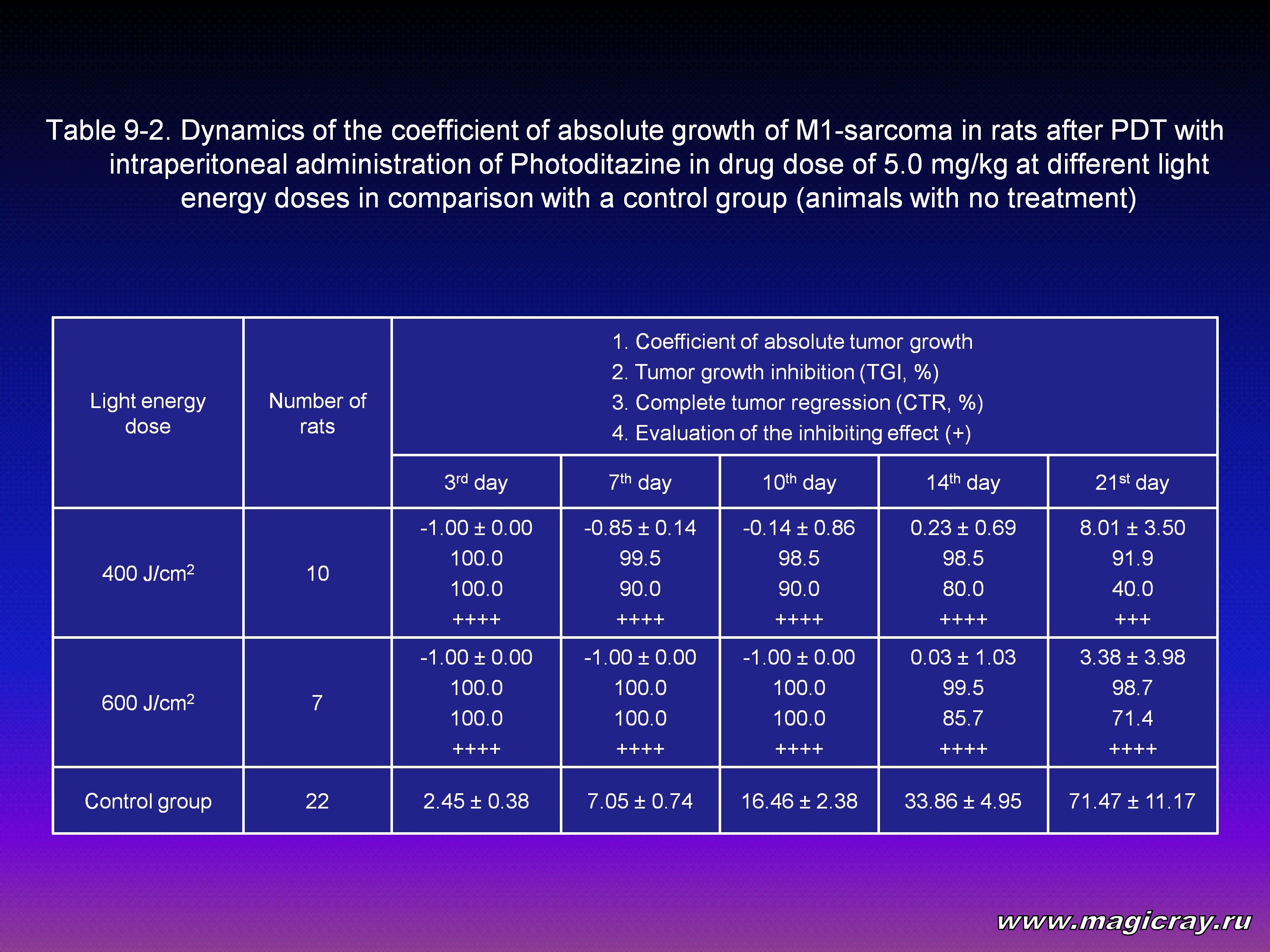
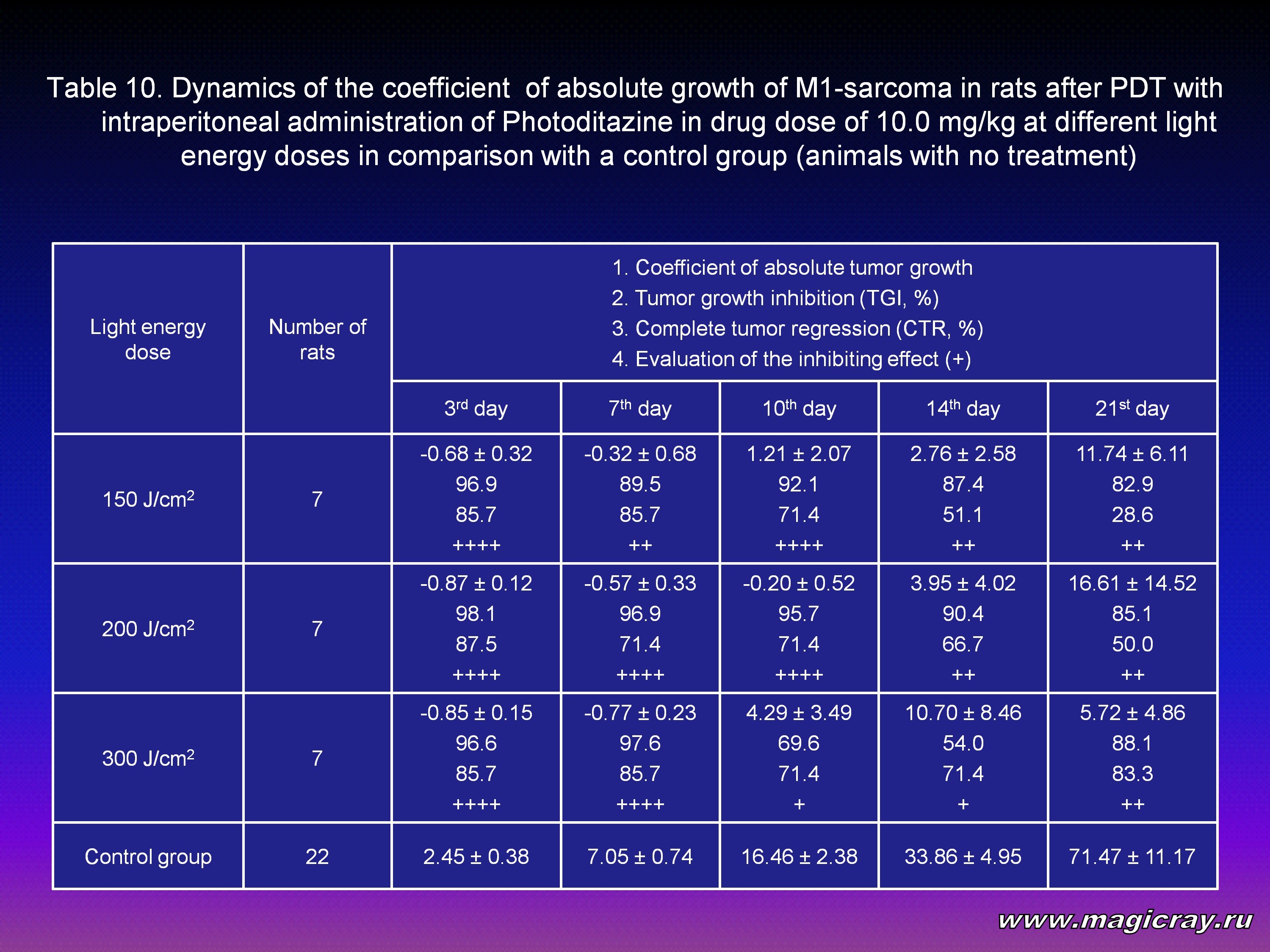
The Tables show that all the given doses of Photoditazine (2.5, 5, 10 mg/kg) and all the light doses (150, 200, 300, 400, 600 J/cm2) on the 21st day after PDT result in significant decrease of the coefficient of absolute tumor growth and certainly a high level of inhibition of its growth. Complete tumor regression in the range from 28.6 % to 83.3 % and the inhibiting effect from + to ++++ can also be seen.
The analysis of the research results shows 5 most effective variants of drug doses and light doses for photodynamic therapy: (2.5 mg/kg; 300 J/cm2); (2.5 mg/kg; 600 J/cm2); (5 mg/kg; 300 J/cm2); (5 mg/kg; 600 J/cm2); (10 mg/kg; 300 J/cm2). If you consider them, the first 4 variants have the same high inhibiting effect (++++) within the whole period of observation (from 3 to 21 days after PDT). The fifth variant (10 mg/kg; 300 J/cm2) shows a higher level of complete tumor regression on the 21st day after PDT (83.3 %), but the level of tumor growth inhibition (88.1 %) doesn’t make it possible to highly estimate the inhibiting effect of this variant. The parameters of tumor growth inhibition and complete tumor regression of M1-sarcoma on the 21st day after PDT are given in Figure 3 and Figure 4.
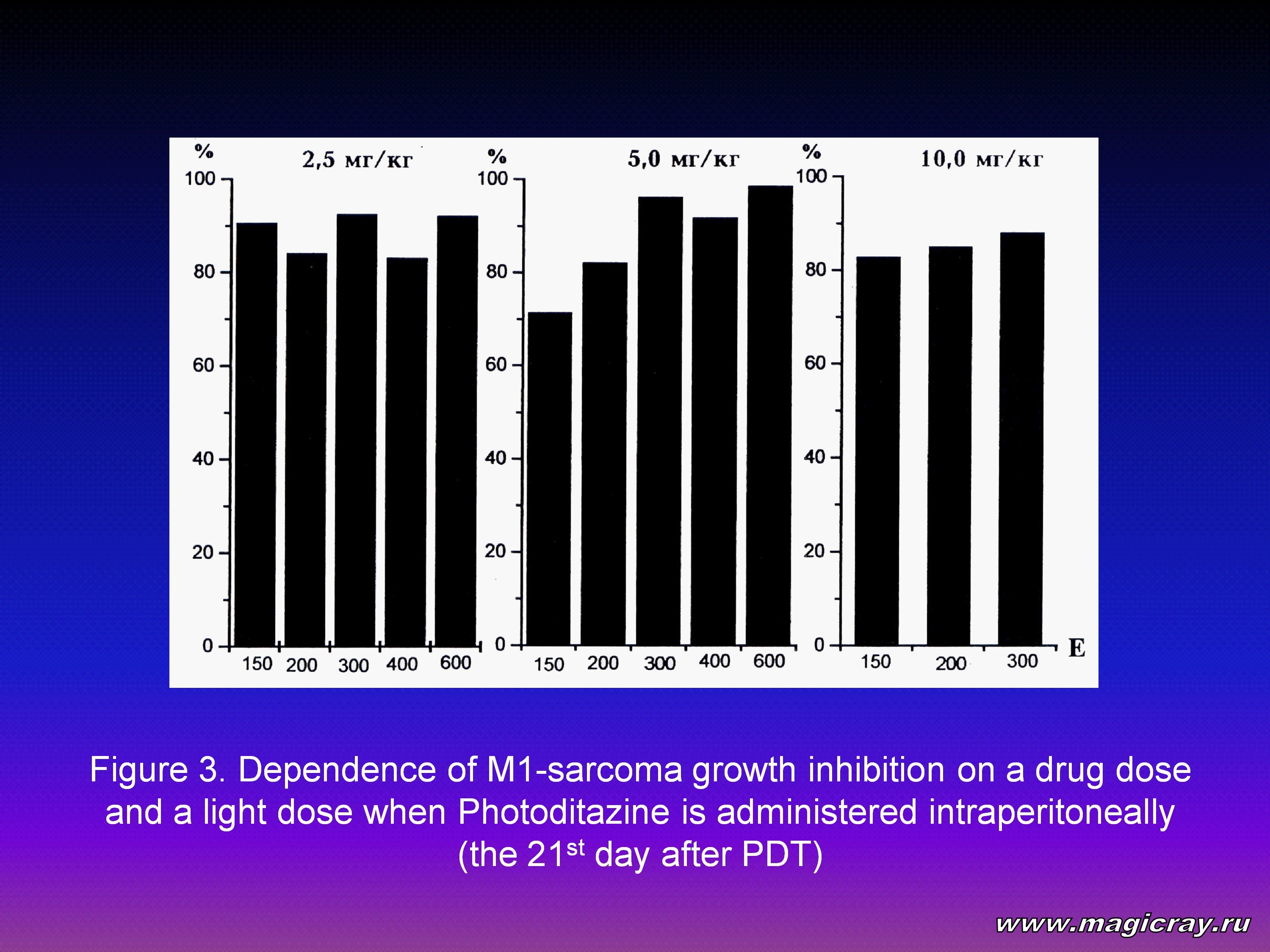
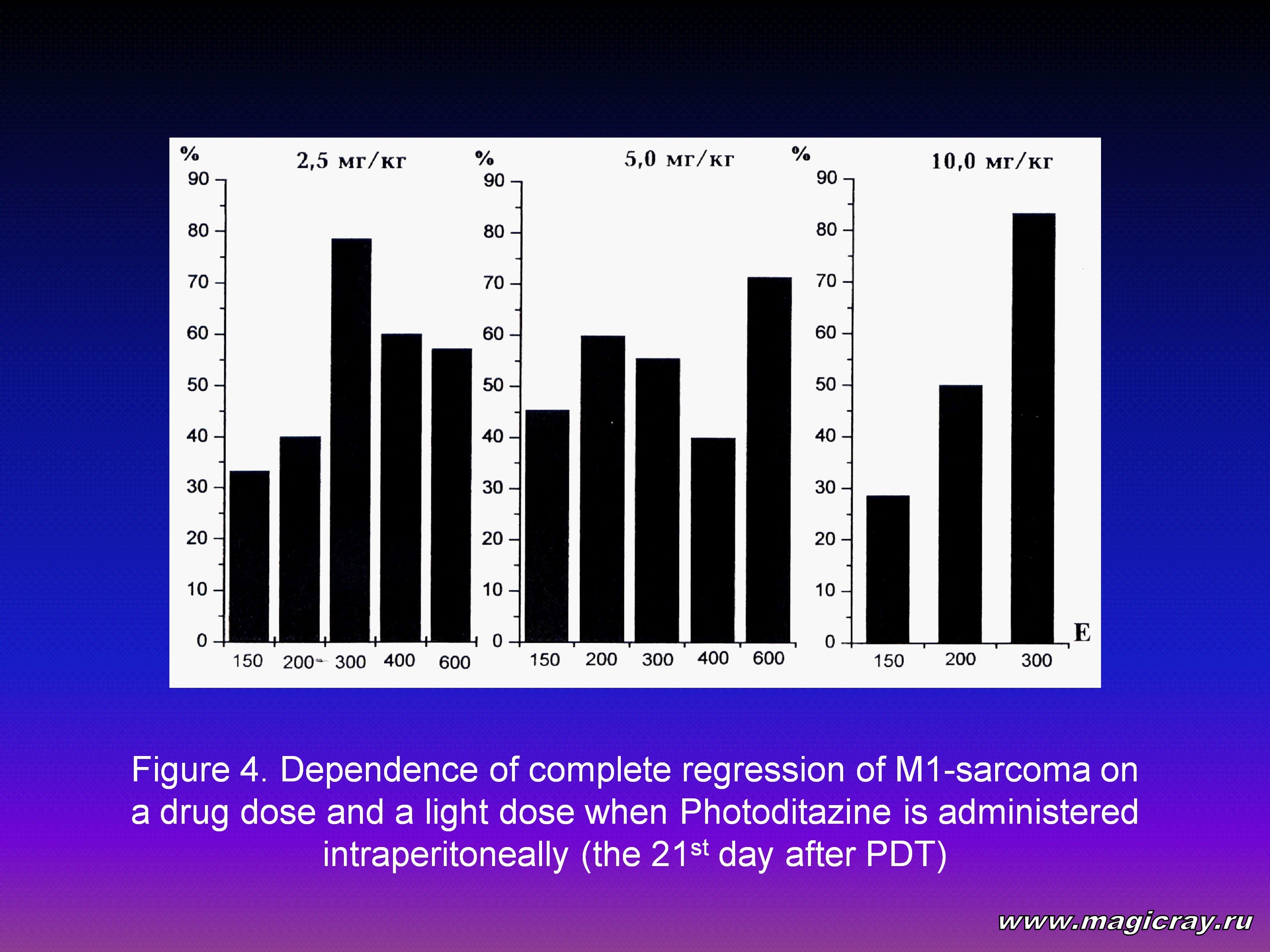
Taking into consideration the given data, we can come to the following conclusions:
1. Photoditazine is a highly effective photosensitizer for photodynamic therapy.
2. The effectivity of Photoditazine depends on a drug dose and a light dose.
3. A more significant antitumoral effect of Photoditazine is shown at drug doses of 2.5 mg/kg, 5 mg/kg and light doses of 300 J/cm2, and 600 J/cm2.
4. The smallest and least effective dose of Photoditazine and light dose (from those analyzed) for PDT are 2.5 mg/kg and 300 J/cm2, respectively.
The first clinical results of PDT with Photoditazine
Photodynamic therapy with Photoditazine was performed in accordance with the two protocols:
1. Primary and recurrent skin cancer.
2. For palliative purposes for recanalization in case with obtrusive cancer of esophagus, cardia, trachea, large bronchi.
Photoditazine was used at doses from 0.3 to 1.5 mg/kg. An average drug dose was 0.8 mg/kg. The minimum effective drug dose was 0.3 mg/kg.
The Crystal 2000 laser semiconductor device (Russia) was used for tumor irradiation with a wavelength of 662 nm and maximum output radiation power of 3 W.
Radiation power density for external irradiation was 0.2 – 0.3 W/cm2, the light dose was 180 – 240 J/cm2. For PDT of internal organs, the light dose was in the range from 75 to 275 J/cm2.
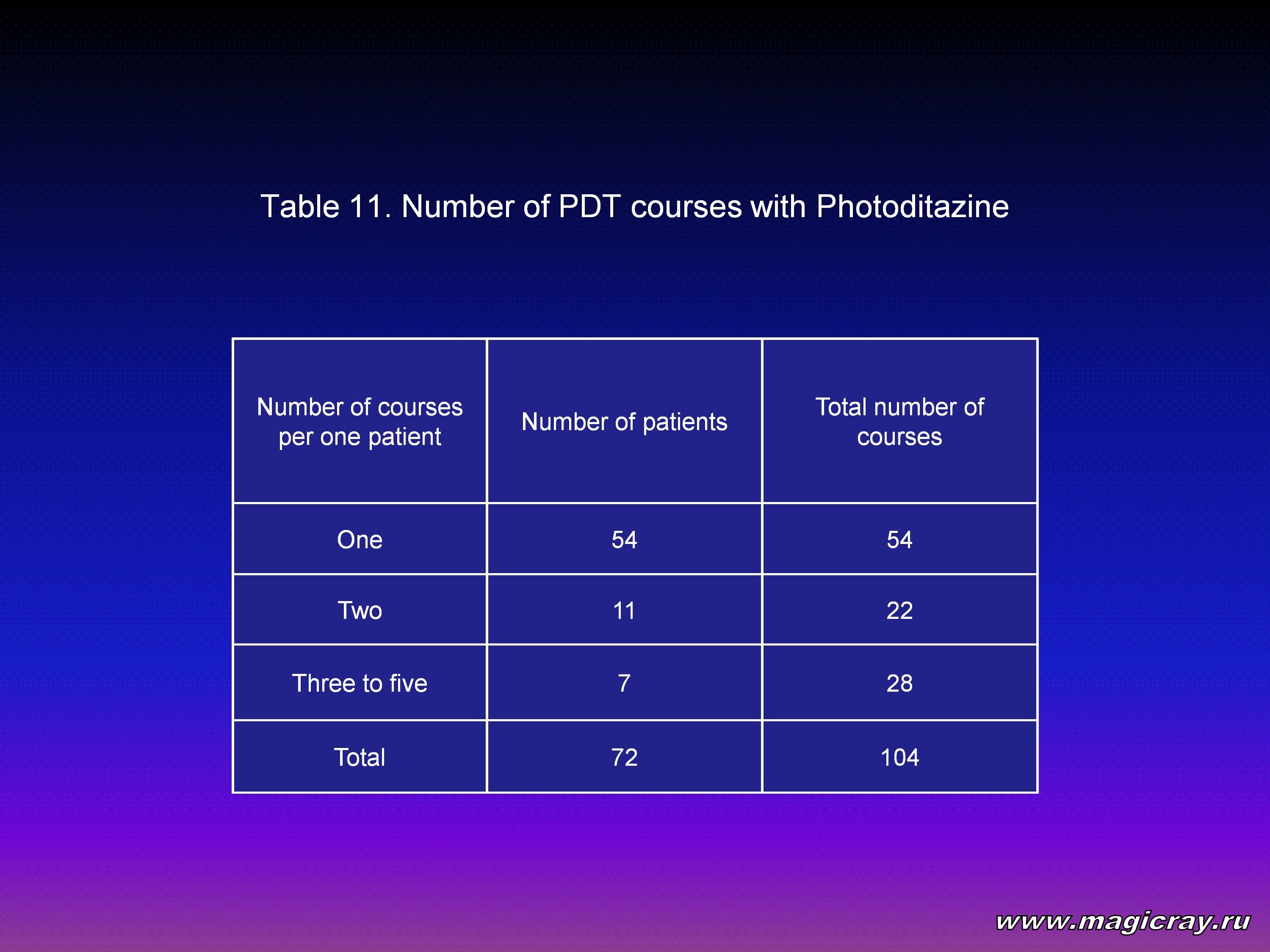
For the purpose of recanalization, PDT was repeated with an interval of 7 – 14 days to achieve staged recanalization of a tubulous organ. From 75 patients (Table 11), 54 patients underwent one PDT course, 11 patients underwent two PDT courses, and 7 patients – 3 – 5 PDT courses. Total 104 PDT courses were performed for 72 patients: 101 courses with intravenous administration of Photoditazine, and 3 courses with intratissual administration of this preparation.
The results were analyzed 2 months later after the treatment in accordance with criteria of the World Health Organization:
1. Conclusion about complete resorption (CR) was made upon absence of visual and palpatory signs of tumor growth, which was also confirmed by negative results of morphological tests.
2. Conclusion about partial resorption (PR) was made upon 50 % decrease of the maximum size of a tumor, and also in case with clinical complete tumor absence, morphological tests detected tumor cells.
3. Decrease of tumor size for less than 50 % or absence of tumor size changes was considered as results with no response (NR).
The results of PDT with Photoditazine are given in Table 12 and Table 13. Complete tumor resorption was achieved in 44 patients, partial – in 28 patients, including 15 patients who underwent PDT for palliative purposes: 12 patients for recanalization of esophagus, cardia, trachea, and bronchi, and 3 patients with advanced cancer of oropharynx and nasopharynx.
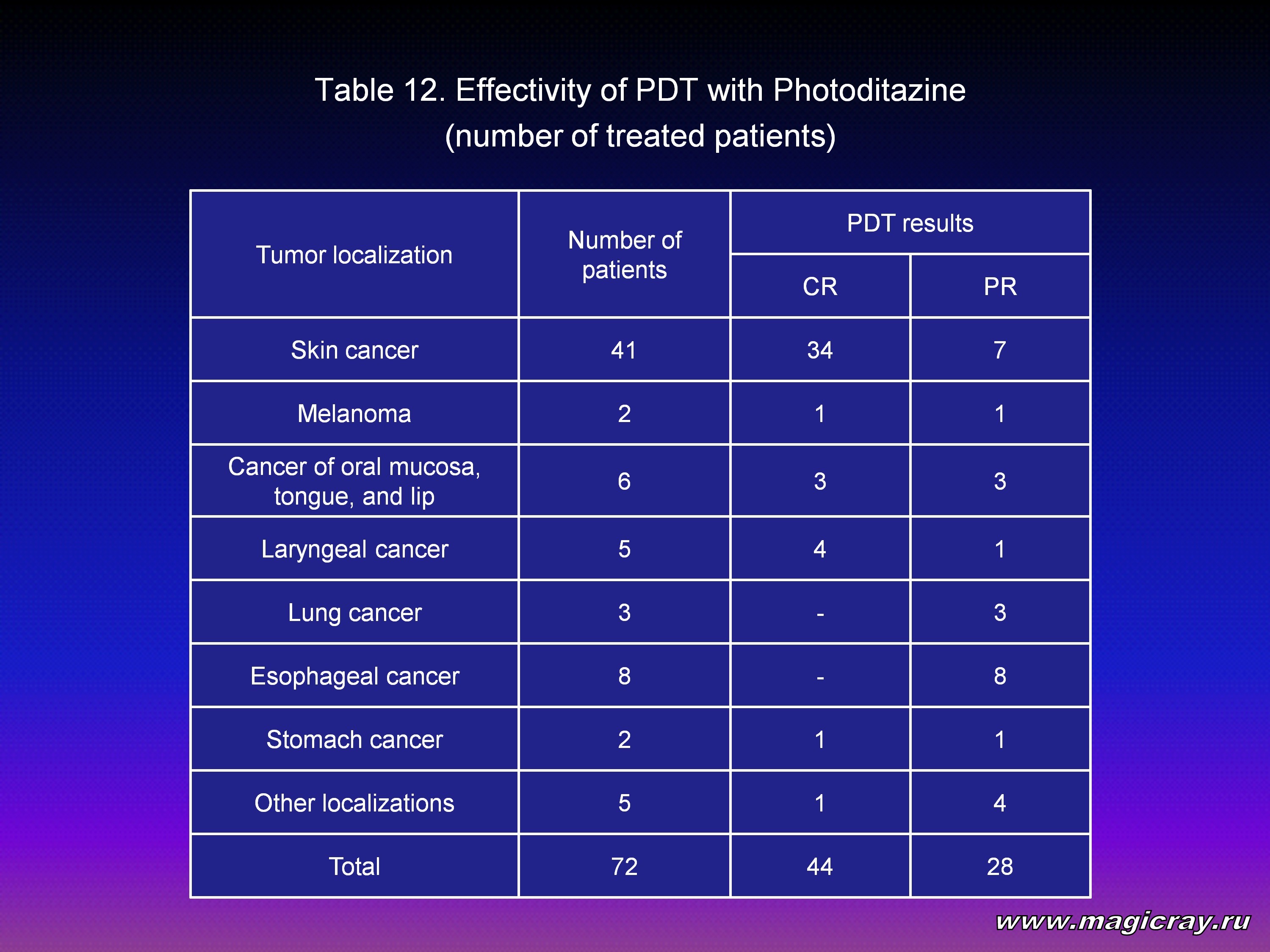
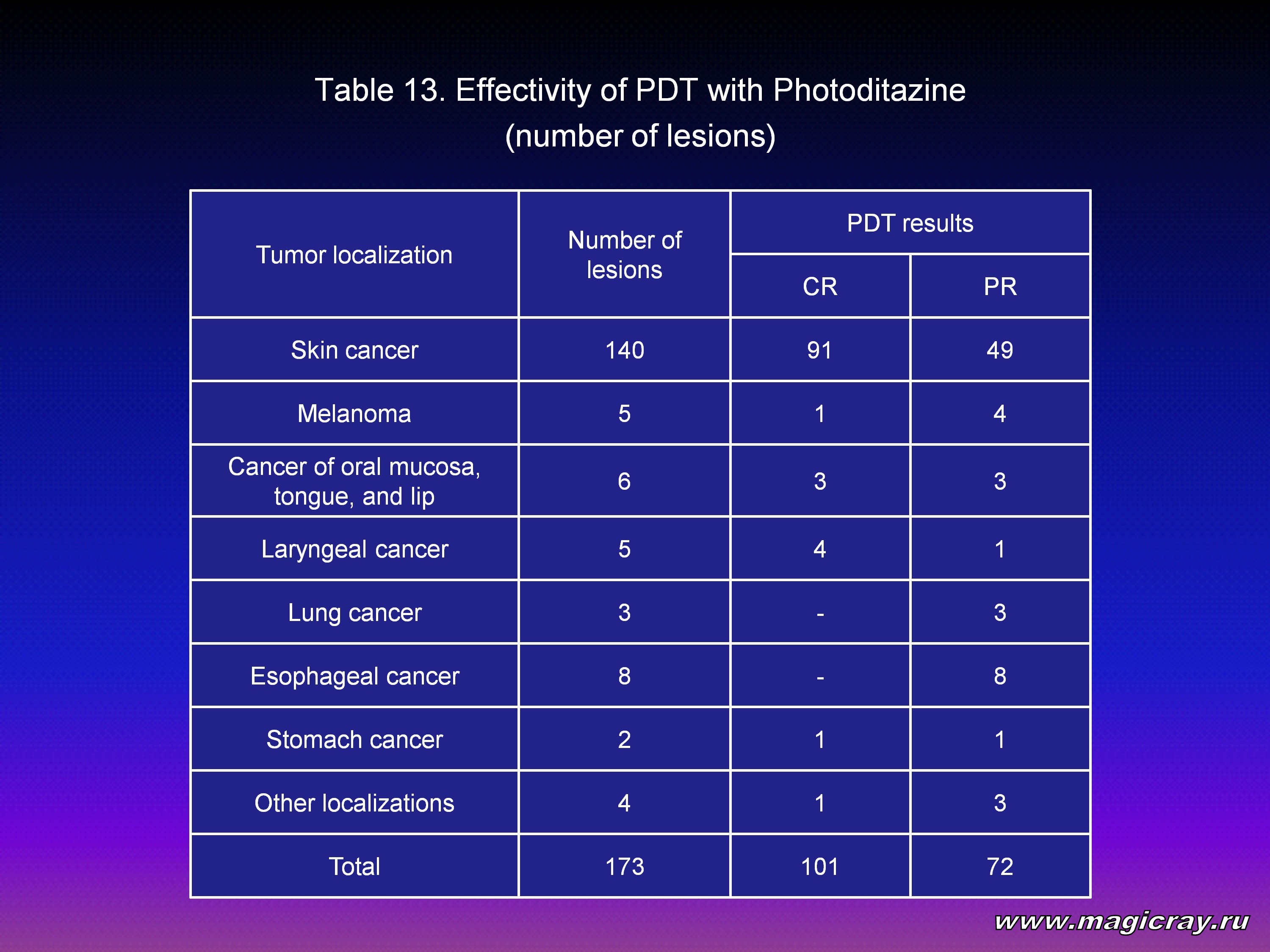
As the Tables show, PDT with Photoditazine led to therapeutic effect in all the cases. There were no cases without any effect. PDT in accordance with the radical program given to patients with primary and recurrent skin cancer caused complete tumor resorption in 82.9 % of cases. Complete resorption after treatment of malignant tumors of larynx was fixed in 80 % of cases.
Palliative PDT for patients with occlusive tumors of internal organs showed a therapeutic effect and the condition of patients improved significantly. PDT for 8 patients with esophageal cancer caused a significant effect of recanalization and recovery of oral feeding. Three of those put on 15 – 20 % of their weight within the first month. The effect of recanalization lasted within 3 – 7 months.
PDT resulted in a strong effect of recanalization with elimination of dyspnea and strident breathing in all the patients with lung cancer on the 3rd to 4th day after the procedure. Control bronchoscopy after the first PDT course showed a partial (50 %) recovery of bronchial lumen, after the 2nd – 3rd PDT course – a complete recovery of bronchial lumen with elimination of hypoventilation and atelectasis which can be detected by X-ray examination and with recovery of lung tissue transparency.
Among the patients with recurrent squamous-cell cancer of tongue and oral mucosa, and recurrent squamous-cell cancer of nasopharynx after radiotherapy, who underwent two PDT courses, one patient had a complete tumor resorption, and two patients – a partial resorption.
After 104 PDT courses there were fixed 20 complications: shiver in 18 patients, including 3 patients with temperature rise up to 38°С, nausea and vomiting; one female patient aged 74 had dizziness and weakness; one patient on the 3rd day after PDT got herpes. Shiver in most patients was slight; it developed 20 – 25 minutes later after the drug administration and lasted from 5 to 30 minutes.
Thus, the data obtained lead us to the following conclusions:
1. Fast elimination of Photoditazine from the body solves the problem of skin phototoxicity which accompanies most photosensitizers used in clinics.
2. Due to fast accumulation in a tumor and high coefficient of contrast between tumorous and normal tissues, Photoditazine reduces the time of treatment from several days to 2 – 3 hours. This property of Photoditazine, along with its high coefficient of contrast and inexpensive portable semiconductor laser devices with a wavelength of 662 nm, makes it an attractive photosensitizer for PDT.
3. PDT with Photoditazine used to treat skin cancer results in a complete tumor resorption in 83 % of patients.
4. PDT with Photoditazine can be used successfully for palliative purposes in patients with an advanced tumor process in esophagus, the proximal part of stomach, trachea, large bronchi, oropharynx and nasopharynx.
Conclusion
Chlorin tetrapyrrol photosensitizers have intensive absorption in long-wavelength region of spectrum, optimal ratio of “fluorescence/interconversion” and show significantly higher light toxicity than most photosensitizers, at that they don’t have simultaneously any dark toxicity. When administered into the body, chlorin photosensitizers show better general toxic properties than porphyrin oligomers or sulfonated phthalocyanines, and the elimination rates of the preparations cannot be compared: Photosense and Photohem remain in the body for more than 3 months while water soluble chlorin photosensitizers – for only 1 to 2 days.
Our structural and functional search enables us to get photosensitizers with good photophysical, bilogical characteristics and high specific activity, which gives an opportunity to make compounds that have a complex of optimal properties for photodynamic therapy.
| 
